Abstract
Ethanol exposure during pregnancy induces cardiac fibrosis in the fetal heart. However, the mechanisms by which consumption of ethanol induces fibrotic changes are not known. Pregnant rats were received ethanol 4.5 g/kg BW once per day from the 7th day of pregnancy (GD7) throughout lactation. Our findings demonstrated that, area of fibrosis increased in cardiac tissue in the pups on both postnatal day twenty one (PN21) and postnatal day ninety (PN90) after prenatal and early postnatal period ethanol treatment compared with the controls. It was accompanied by a decline in the expression of SIRT1 protein along with the elevation of FOXO3a and TGF-β protein expressions which were determined by western blot. Overall, our data reveal that prenatal alcohol usage increase in fibrotic regions in the pup hearts possibly by regulating TGF-β, FOXO3a and SIRT1 protein levels. These are potential therapeutic molecular targets that can be modulated to protect heart against maternal ethanol exposure.



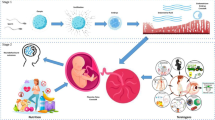
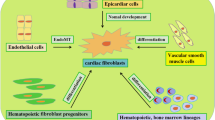
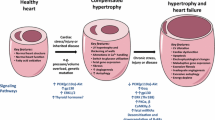
Similar content being viewed by others
Data Availability
The datasets generated during and/or analyzed during this study are available from the corresponding author on reasonable request.
References
Jones, K. L., & Smith, D. W. (1973). Recognition of the fetal alcohol syndrome in early infancy. Lancet (London, England), 302(7836), 999–1001.
Henderson, G. I., Devi, B. G., Perez, A., & Schenker, S. (1995). In utero ethanol exposure elicits oxidative stress in the rat fetus. Alcoholism, Clinical and Experimental Research, 19(3), 714–720.
Daft, P. A., Johnston, M. C., & Sulik, K. K. (1986). Abnormal heart and great vessel development following acute ethanol exposure in mice. Teratology, 33(1), 93–104.
Shirpoor, A., Gaderi, R., & Naderi, R. (2019). Ethanol exposure in prenatal and early postnatal induced cardiac injury in rats: Involvement of oxidative stress, Hsp70, ERK 1/2, JNK, and apoptosis in a 3-month follow-up study. Cell Stress & Chaperones, 24(5), 917–926.
Patel, V. B., Why, H. J., Richardson, P. J., & Preedy, V. R. (1997). The effects of alcohol on the heart. Adverse Drug Reactions and Toxicological Reviews, 16(1), 15–43.
Piano, M. R., & Phillips, S. A. (2014). Alcoholic cardiomyopathy: Pathophysiologic insights. Cardiovascular Toxicology, 14(4), 291–308.
Zhou, C., Huang, J., Li, Q., Zhan, C., He, Y., Liu, J., et al. (2018). Pharmacological inhibition of soluble epoxide hydrolase ameliorates chronic ethanol-Induced cardiac fibrosis by restoring autophagic flux. Alcoholism, Clinical and Experimental Research, 42(10), 1970–1978.
Ma, Z., Zang, W., Wang, H., & Wei, X. (2020). Silibinin enhances anti-renal fibrosis effect of MK-521 via downregulation of TGF-β signaling pathway. Human Cell, 33(2), 330–336.
Gaitantzi, H., Meyer, C., Rakoczy, P., Thomas, M., Wahl, K., Wandrer, F., et al. (2018). Ethanol sensitizes hepatocytes for TGF-β-triggered apoptosis. Cell Death & Disease, 9(2), 51.
Uesugi, T., Froh, M., Gäbele, E., Isayama, F., Bradford, B. U., Ikai, I., et al. (2004). Contribution of angiotensin II to alcohol-induced pancreatic fibrosis in rats. The Journal of Pharmacology and Experimental Therapeutics, 311(3), 921–928.
Singhal, P. C., Reddy, K., Ding, G., Kapasi, A., Franki, N., Ranjan, R., et al. (1999). Ethanol-induced macrophage apoptosis: The role of TGF-beta. Journal of Immunology, 162(5), 3031–3036.
Law, B. A., & Carver, W. E. (2013). Activation of cardiac fibroblasts by ethanol is blocked by TGF-β inhibition. Alcoholism, Clinical and Experimental Research, 37(8), 1286–1294.
Alcendor, R. R., Gao, S., Zhai, P., Zablocki, D., Holle, E., Yu, X., et al. (2007). Sirt1 regulates aging and resistance to oxidative stress in the heart. Circulation Research, 100(10), 1512–1521.
Ninh, V. K., El Hajj, E. C., Ronis, M. J., & Gardner, J. D. (2019). N-Acetylcysteine prevents the decreases in cardiac collagen I/III ratio and systolic function in neonatal mice with prenatal alcohol exposure. Toxicology Letters, 315, 87–95.
Pulla, V. K., Battu, M. B., Alvala, M., Sriram, D., & Yogeeswari, P. (2012). Can targeting SIRT-1 to treat type 2 diabetes be a good strategy? A review. Expert Opinion on Therapeutic Targets, 16(8), 819–832.
Yang, J., Wang, N., Zhu, Y., & Feng, P. (2011). Roles of SIRT1 in high glucose-induced endothelial impairment: Association with diabetic atherosclerosis. Archives of Medical Research, 42(5), 354–360.
Xie, J., Zhang, X., & Zhang, L. (2013). Negative regulation of inflammation by SIRT1. Pharmacological Research, 67(1), 60–67.
Samuel, S. M., Thirunavukkarasu, M., Penumathsa, S. V., Paul, D., & Maulik, N. (2008). Akt/FOXO3a/SIRT1-mediated cardioprotection by n-tyrosol against ischemic stress in rat in vivo model of myocardial infarction: Switching gears toward survival and longevity. Journal of Agricultural and Food Chemistry, 56(20), 9692–9698.
Brunet, A., Sweeney, L. B., Sturgill, J. F., Chua, K. F., Greer, P. L., Lin, Y., et al. (2004). Stress-dependent regulation of FOXO transcription factors by the SIRT1 deacetylase. Science (New York, NY), 303(5666), 2011–2015.
Langley, E., Pearson, M., Faretta, M., Bauer, U. M., Frye, R. A., Minucci, S., et al. (2002). Human SIR2 deacetylates p53 and antagonizes PML/p53-induced cellular senescence. The EMBO Journal, 21(10), 2383–2396.
Yeung, F., Hoberg, J. E., Ramsey, C. S., Keller, M. D., Jones, D. R., Frye, R. A., et al. (2004). Modulation of NF-kappaB-dependent transcription and cell survival by the SIRT1 deacetylase. The EMBO Journal, 23(12), 2369–2380.
Motta, M. C., Divecha, N., Lemieux, M., Kamel, C., Chen, D., Gu, W., et al. (2004). Mammalian SIRT1 represses forkhead transcription factors. Cell, 116(4), 551–563.
Huang, H., & Tindall, D. J. (2007). Dynamic FoxO transcription factors. Journal of Cell Science, 120(Pt 15), 2479–2487.
Tzivion, G., Dobson, M., & Ramakrishnan, G. (2011). FoxO transcription factors; Regulation by AKT and 14-3-3 proteins. Biochimica et Biophysica Acta, 1813(11), 1938–1945.
Zhang, B., Turdi, S., Li, Q., Lopez, F. L., Eason, A. R., Anversa, P., et al. (2010). Cardiac overexpression of insulin-like growth factor 1 attenuates chronic alcohol intake-induced myocardial contractile dysfunction but not hypertrophy: Roles of Akt, mTOR, GSK3beta, and PTEN. Free Radical Biology & Medicine, 49(7), 1238–1253.
Mohaddes, G., Abdolalizadeh, J., Babri, S., & Hossienzadeh, F. (2017). Ghrelin ameliorates blood-brain barrier disruption during systemic hypoxia. Experimental Physiology, 102(3), 376–382.
Shirpoor, A., Nemati, S., Ansari, M. H., & Ilkhanizadeh, B. (2015). The protective effect of vitamin E against prenatal and early postnatal ethanol treatment-induced heart abnormality in rats: A 3-month follow-up study. International Immunopharmacology, 26(1), 72–79.
Huynh, K. (2014). Risk factors. Reducing alcohol intake improves heart health. Nature Reviews Cardiology, 11(9), 495.
Lluís, M., Fernández-Solà, J., Castellví-Bel, S., Sacanella, E., Estruch, R., & Urbano-Márquez, A. (2011). Evaluation of myocyte proliferation in alcoholic cardiomyopathy: Telomerase enzyme activity (TERT) compared with Ki-67 expression. Alcohol and Alcoholism (Oxford, Oxfordshire), 46(5), 534–541.
Shirpoor, A., Norouzi, L., Khadem-Ansari, M. H., Ilkhanizadeh, B., & Karimipour, M. (2014). The protective effect of vitamin E on morphological and biochemical alteration induced by pre and postnatal ethanol administration in the testis of male rat offspring: A three months follow-up study. Journal of Reproduction & Infertility, 15(3), 134–141.
Lan, N., Yamashita, F., Halpert, A. G., Ellis, L., Yu, W. K., Viau, V., et al. (2006). Prenatal ethanol exposure alters the effects of gonadectomy on hypothalamic-pituitary-adrenal activity in male rats. Journal of Neuroendocrinology, 18(9), 672–684.
Weinberg, J., Kim, C. K., & Yu, W. (1995). Early handling can attenuate adverse effects of fetal ethanol exposure. Alcohol (Fayetteville, NY), 12(4), 317–327.
Lan, N., Vogl, A. W., & Weinberg, J. (2013). Prenatal ethanol exposure delays the onset of spermatogenesis in the rat. Alcoholism, Clinical and Experimental Research, 37(7), 1074–1081.
Fakoya, F. A., & Caxton-Martins, E. A. (2004). Morphological alterations in the seminiferous tubules of adult Wistar rats: The effects of prenatal ethanol exposure. Folia Morphologica, 63(2), 195–202.
Lajiness, J. D., & Conway, S. J. (2012). The dynamic role of cardiac fibroblasts in development and disease. Journal of Cardiovascular Translational Research, 5(6), 739–748.
Bao, M. W., Cai, Z., Zhang, X. J., Li, L., Liu, X., Wan, N., et al. (2015). Dickkopf-3 protects against cardiac dysfunction and ventricular remodelling following myocardial infarction. Basic Research in Cardiology, 110(3), 25.
Li, H., Cai, H., Deng, J., Tu, X., Sun, Y., Huang, Z., et al. (2018). TGF-β-mediated upregulation of Sox9 in fibroblast promotes renal fibrosis. Biochimica et Biophysica acta Molecular Basis of Disease, 1864(2), 520–532.
Higgins, S. P., Tang, Y., Higgins, C. E., Mian, B., Zhang, W., Czekay, R. P., et al. (2018). TGF-β1/p53 signaling in renal fibrogenesis. Cellular Signalling, 43, 1–10.
Xiao, J., Sheng, X., Zhang, X., Guo, M., & Ji, X. (2016). Curcumin protects against myocardial infarction-induced cardiac fibrosis via SIRT1 activation in vivo and in vitro. Drug Design, Development and Therapy, 10, 1267–1277.
March, J. T., Golshirazi, G., Cernisova, V., Carr, H., Leong, Y., Lu-Nguyen, N., et al. (2018). Targeting TGFβ signaling to address fibrosis using antisense oligonucleotides. Biomedicines, 6(3), 74.
Michishita, E., Park, J. Y., Burneskis, J. M., Barrett, J. C., & Horikawa, I. (2005). Evolutionarily conserved and nonconserved cellular localizations and functions of human SIRT proteins. Molecular Biology of the Cell, 16(10), 4623–4635.
Liu, Z. H., Zhang, Y., Wang, X., Fan, X. F., Zhang, Y., Li, X., et al. (2019). SIRT1 activation attenuates cardiac fibrosis by endothelial-to-mesenchymal transition Biomedicine & pharmacotherapy. Biomedecine & Pharmacotherapie, 118, 109227.
Asadi-Azarbaijani, B., Braber, S., van Duursen, M., Jahnukainen, K., Santos, R., & Oskam, I. (2019). Imatinib mesylate does not counteract ovarian tissue fibrosis in postnatal rat ovary. Reproductive Biology, 19(2), 133–138.
Lin, C. H., Lin, C. C., Ting, W. J., Pai, P. Y., Kuo, C. H., Ho, T. J., et al. (2014). Resveratrol enhanced FOXO3 phosphorylation via synergetic activation of SIRT1 and PI3K/Akt signaling to improve the effects of exercise in elderly rat hearts. Age (Dordrecht, Netherlands), 36(5), 9705.
Ni, H. M., Du, K., You, M., & Ding, W. X. (2013). Critical role of FoxO3a in alcohol-induced autophagy and hepatotoxicity. The American Journal of Pathology, 183(6), 1815–1825.
Lai, L., Yan, L., Gao, S., Hu, C. L., Ge, H., Davidow, A., et al. (2013). Type 5 adenylyl cyclase increases oxidative stress by transcriptional regulation of manganese superoxide dismutase via the SIRT1/FoxO3a pathway. Circulation, 127(16), 1692–1701.
Kwak, H. B., Lee, Y., Kim, J. H., Van Remmen, H., Richardson, A. G., & Lawler, J. M. (2015). MnSOD overexpression reduces fibrosis and pro-apoptotic signaling in the aging mouse heart. The Journals of Gerontology Series A, Biological Sciences and Medical Sciences, 70(5), 533–544.
Li, K., Zhai, M., Jiang, L., Song, F., Zhang, B., Li, J., et al. (2019). Tetrahydrocurcumin ameliorates diabetic cardiomyopathy by attenuating high glucose-induced oxidative stress and fibrosis via activating the SIRT1 pathway. Oxidative Medicine and Cellular Longevity, 2019, 6746907.
Zhou, L., Li, P., Zhang, M., Han, B., Chu, C., Su, X., et al. (2020). Carbon black nanoparticles induce pulmonary fibrosis through NLRP3 inflammasome pathway modulated by miR-96 targeted FOXO3a. Chemosphere, 241, 125075.
Ni, Y., Deng, J., Liu, X., Li, Q., Zhang, J., Bai, H., et al. (2021). Echinacoside reverses myocardial remodeling and improves heart function via regulating SIRT1/FOXO3a/MnSOD axis in HF rats induced by isoproterenol. Journal of Cellular and Molecular Medicine, 25(1), 203–216.
Acknowledgements
This study was supported by school of medicine, Urmia University of Medical Sciences, Urmia, Iran.
Author information
Authors and Affiliations
Contributions
AS: Data curation., Methodology., Writing—review & editing. RN: Conceptualization., Formal analysis., Methodology., Project administration., Supervision., Validation., Visualization., Writing—original draft., Writing—review & editing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Handling Editor: Y. James Kang.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shirpoor, A., Naderi, R. Maternal Ethanol Exposure-Induced Cardiac Fibrosis is Associated with Changes in TGF-β and SIRT1/FOXO3a Signaling in Male Rat Offspring: A Three-Month Follow-up Study. Cardiovasc Toxicol 22, 858–865 (2022). https://doi.org/10.1007/s12012-022-09761-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12012-022-09761-7